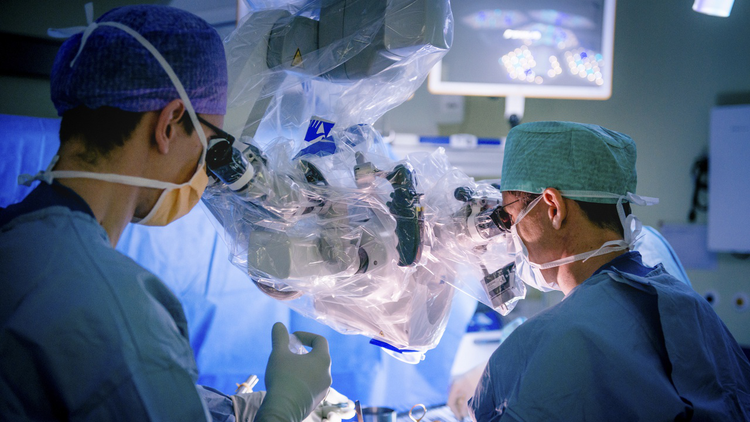
Brain tumor surgery is pretty advanced and fancy these days. There are many technologies that help the neurosurgeon operate accurately without harming normal brain tissue. Such technologies include microscopy, neuro-navigation, intraoperative contrast enhancement, intraoperative magnetic resonance imaging (MRI), neurophysiological monitoring, intraoperative ultrasound, awake surgery and many others.
Unfortunately, nature has come up with a group of brain tumors that can neither be recognized with the naked eye nor with a microscope during surgery. Those tumors are particularly similar to normal brain tissue and are more challenging to operate on. If the tumor resection is incomplete the patient might suffer from earlier recurrence and shorter survival. If the resection is too large the patient might have serious neurological deficits after surgery.
In its cellular structure and composition, the tumor is very much different from the brain, though. Brain cells have a very tidy arrangement and they form brain fibers that run a very precise and predetermined course. The tumor on the other hand, consists of a pile of erratic and nonfunctional cells. How come we can see it so easily if we look at the single cell but can’t recognize the tumor while we operate? Where is the bigger picture? This is why the challenge is named HORAO, the Greek word for “seeing with the mind”.
But, this has nothing to do with supernatural powers or fortune telling. The HORAO Challenge aims to improve brain surgery with the help of a technology that visualizes brain fibers. The Challenge seeks an idea. We welcome entrepreneurs, researchers, scientists, engineers, students, and anyone eager to contribute, to search for a solution. We believe that the solution is already out there and just needs to be found and implemented. If this project succeeds it will have the power to improve brain tumor survival in a population of millions of young patients with a devastating disease.
In order to make the HORAO Challenge possible, people around the world have contributed to one of the first successful neuroscience crowdfunding campaign: Their donation is your prize money!
The challenge is run by a group of inspired neurosurgeons at the Inselspital, Bern University Hospital, Switzerland in Europe.
What Can You Do Right Now?
- Click ACCEPT CHALLENGE above to sign up for the challenge.
- Read the Challenge Guidelines to learn about the requirements and rules.
- Share this challenge on social media using the icons above. Show your friends, your family, or anyone you know who has a passion for discovery.
- Start a conversation in our Forum to join the conversation, ask questions or connect with other innovators.
The Problem
The following text is also available as PDF: Guidelines (PDF)
- Brain tumors have a devastating effects on patients and their relatives.
- For obvious reasons, brain surgery better be exact.
- Brain tumors look very similar to the normal brain, and can often not be discerned.
- Brain tissue consist of orderly fibers, whereas tumor tissue is chaotic. This difference in structure could be used to differentiate tumor from brain tissue.
- However, the fibers and their structures can not yet be seen non-invasively during surgery.
The Human Brain
The human brain is a vital organ responsible for motion, intelligence, memory, sensation, thought, speech and emotion of a human being. It is the key to our mind and soul without which a human cannot exist. Together with the spinal cord it is part of the central nervous system and is located in the skull. The human brain makes up 2 % of the body weight and consumes 20 % of total body energy. It contains about 90 billion nerve cells, called neurons, and around the same number of supporting cells called glial cells.
The cellular body of a neuron is located in the so-called gray matter at the very surface of the brain. The extension of a neuron, called axon or nerve fiber, connects different parts of the brain and spinal cord with trillions of synapses and makes up the white matter. Thousands and millions of nerve fibers of similar function run in bundles and are called fiber tracts. Fiber tracts always run in a predetermined way and may be many inches long.
Different brain functions are based in different areas. For example, production of speech is located in the front part of the brain while vision is located in the back part. Brain areas that house vital functions like speech, movement, memory or vision are called eloquent, while areas of no particular significance are called non-eloquent.
Tumors of the Brain and How to Treat Them
Brain tumors can occur at any age but most frequently affect children and older adults. The word tumor is used synonymous to cancer and is per definition the abnormal and uncontrolled growth of tissue that usually forms a mass. Primary brain tumors originate from brain tissue, while metastatic brain tumors begin in any given organ and then spread to the brain. Classified by their growth behavior tumors can either be benign, malignant or something in between. Benign tumors grow slowly and never spread to different tissue. Malignant tumors tend to grow very fast, destroy their surroundings and can spread elsewhere.
The most common primary brain tumor is the glioma. It arises from the glial cells, which are responsible for the support and cohesion of the neurons. Gliomas grow from within the brain and infiltrate the surrounding tissue. The malignant form of the glioma is called glioblastoma and is the most common primary malignant brain tumor in adulthood. Low grade gliomas on the other hand are tumors that grow slower, are more adapted to the brain, less destructive and therefore less distinguishable from the normal brain than a glioblastoma. However, they equally infiltrate the surrounding tissue and are thus neither benign nor malignant in terms of conventional definition.
If growing in a non-eloquent area gliomas can remain unnoticed for a very long time especially, which is often the case in low-grade of young patients. When diagnosed, the first treatment step is to remove the glioma through surgery. The surgical excision of as much of the glioma as possible is crucial to improve survival of the patient. Radiation and chemotherapy are often used to delay recurrence of the tumor.
Challenges of Brain Tumor Surgery
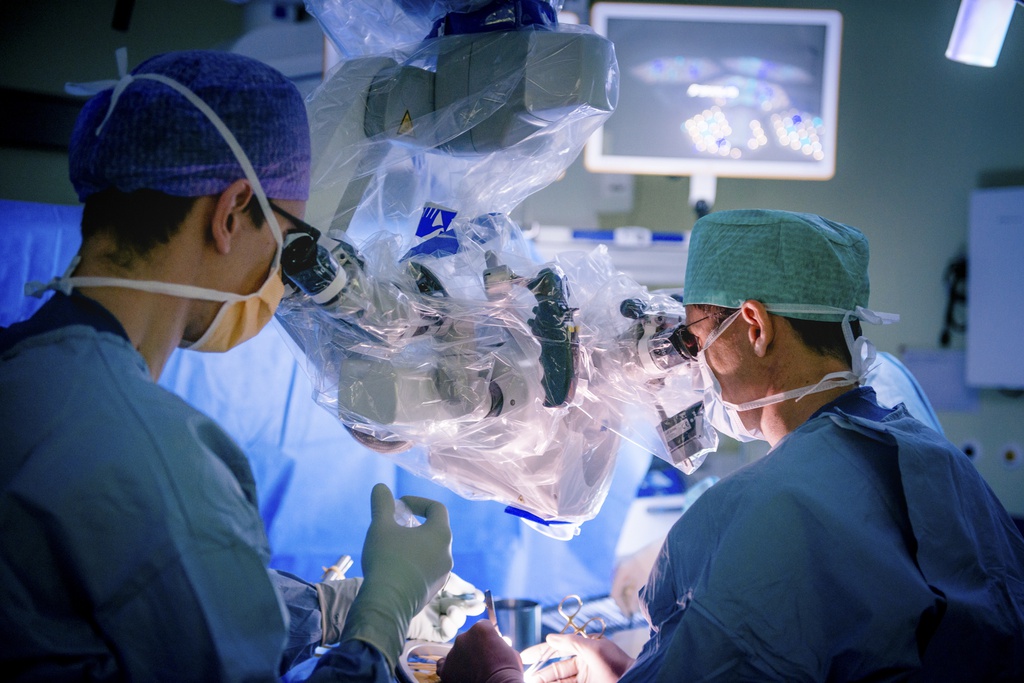
Most brain tumor surgery is done under general anaesthesia. Tumors close to brain areas responsible for speech or vision may require the patient to be awake in order to check the exact location of these important brain functions. The surgeons use a large, free floating binocular operation microscope that magnifies the operation site. The microscope is the surgeon’s most important ally, as it enables him to see structures more accurately, and beyond his normal vision.
Despite these abilities the microscope does not help the surgeon to distinguish between healthy brain and brain tumor. In contrast to the high organizational level of cells and fiber geometry in the brain, the appearance of brain tissue under the microscope is quite plain. The tissue appears mostly soft (like firm jelly) and is white, while the top inch at the surface of the brain is gray, hence the terms white and gray matter as mentioned above. Especially gliomas, which are originating from the brain cells themselves, look just like brain tissue. The surgeon often struggles to see the border between the brain and the tumor even under the microscope. This problem is particularly evident in low grade gliomas which infiltrate the brain and look almost exactly like healthy brain tissue.
The most important goal of surgery is to remove as much tumor as possible without harming important brain functions. An overlooked rim of only 1 or 2 millimeters of tumor may lead to early recurrence of the tumor and reduced survival time; however, important brain areas may irreversibly be damaged if the surgeon removes 1 or 2 millimeters too much, causing devastating harm to the patient.
Three different techniques (Neuronavigation, Neuromonitoring, 5-ALA) are being used at present to aid the surgeon in finding tumor borders. But these techniques are either only estimates of the tumor borders and therefore not adequate for the high requirements of the surgery, or are only applicable in some brain tumors.
Why Does this Problem Exist?
In the quest to improve brain tumor surgery, most scientists have focused on directly visualizing tumors. Nonetheless, despite years of research on direct visualization, this strategy has failed for most types of brain tumors.
The Challenge Breakthrough
A solution to the HORAO challenge would fundamentally change todays brain surgery by providing the surgeon with real time visualization of the brains microarchitecture. It would unveil subtle differences between the human brain tissue and certain diseases yet hidden to the human eye. A challenge breakthrough would improve current surgical strategies at their base with a substantial, worldwide impact on patient safety and outcome.
We believe that in today's interconnected world of endless translational research possibilities the time is right for a solution to the HORAO challenge.
Our Commitment to a Solution
To understand the HORAO project, we have to take a step backwards: in 2017, we – a group of inspired neurosurgeons from the Inselspital, Bern University Hospital – initiated the ambitious project. We launched a crowdfunding campaign in order to make brain tumor surgery safer. It was to become one of the first successful neuroscience crowdfunding projects worldwide. Right from the start, our goal was to launch a crowdsourcing campaign as a second step, because we are convinced that there is a solution to our problem – perhaps it already exists. On March 14, 2019 up to five competitors will be invited to the HORAO Conference in Bern, Switzerland. Only then will it be decided who will win the HORAO Challenge. The conference will be attended by our jury, donors, practicing neurosurgeons, researchers, opticians, developers, and manufacturers of medical technology, which will provide a rich infrastructure and ecosystem of support for those invited to present.

Prize
| 1st prize | $35,000 |
| 2nd prize | $12,000 |
| 3rd–5th prizes | $1,000 |
Up to five finalists are invited to join the final round at the HORAO Conference and convince the jury and the public of their project. The conference will be held on March 14, 2019 as a part of the Brainweek Bern in Bern, Switzerland. Finalists must present at the conference in order to compete for the prize. Travel and hotel expenses for one overnight stay will be paid for by the HORAO Challenge.
Timeline
| Pre-registration begins: | April 24th, 2018 |
| Open to submissions: | June 12th, 2018 |
| Submission deadline: | November 16th, 2018 @ 5pm ET |
| Judging: | December 1st, 2018 to January 7th, 2019 |
| Winner Announcement: | January 15th, 2019 |
| Finals (up to five participants): | March 14th, 2019 |
Judging Criteria
The jury assesses all submission based on the Pre-Round Judging Criteria. Up to five finalists are determined by the pre-round scores and subsequently invited to the final round. The pre-round technical judging criteria constitutes 50 % of the final score. The other 50 % is based on the presentation, content and feasibility, as judged by the jury and the public during the HORAO Conference.
Pre-Round Technical Judging Criteria
| Section | Description | Overall Weight |
|---|
| Detection of cerebral tissue | The solution discerns brain from tumor tissue. | 20 |
|---|
| Detection of fiber tracts | The solution detects brain tissue in such a way that the spatial orientation of fiber tracts can be seen. | 20 |
|---|
| Real time detection | Time used for visualization must be short (minutes), in order not to disrupt the flow of surgery. | 20 |
|---|
| Size of the solution | The size of the solution must be such that it fits well into an operating theater (not larger than 2 cubic meter). | 10 |
|---|
| Non-invasiveness | The solution must not harm or remove the investigated tissue. | 20 |
|---|
| Repetitiveness | The solution must be able to be used repetitively at short interval (minutes). | 10 |
|---|
Final Round Judging Criteria
| Section | Description | Overall Weight |
|---|
| Score of Pre-Round | The total score obtained in the pre-round accounts for 50 % of the final score. The Jury will not communicate the Pre-Round Score. | 50 |
|---|
| Presentation, content and feasibility by jury | The jurors judge presentation, content and feasibility. | 25 |
|---|
| Presentation, content and feasibility by public vote | The public at the conference judge presentation, content and feasibility. | 25 |
|---|
How Do I Win?
To be eligible for an award, your proposal must, at minimum:
- Satisfy the Judging Scorecard requirements.
- Thoughtfully address the Submission Form questions.
- Up to five top-scores are winners, and will be invited to the finals in Switzerland!
Solutions must, at a minimum:
- Help to distinguish brain tissue from tumor tissue, or:
- Identify large fiber tracts.
Rules
Participation Eligibility
The challenge is open to all adult individuals, private teams, public teams, and collegiate teams. Teams may originate from any country. Submissions must be made in English. All challenge-related communication will be in English.
No specific qualifications or expertise in the field of neurosurgery or medicine is required. Prize organizers encourage outside individuals and non-expert teams to compete and propose new solutions.
To be eligible to compete, you must comply with all the terms of the challenge as defined in the Challenge-Specific Agreement.
Registration and Submissions
Submissions must be made online (only), via upload to the HeroX.com website, on or before 5pm ET, November 16th, 2018. All uploads must be in PDF format. No late submissions will be accepted.
Intellectual Property Rights
As detailed in the Challenge-Specific Agreement, competitors will retain all intellectual property rights to their technology.
Selection of Winners
Based on the winning criteria, prizes will be awarded per the Judging Criteria section above. In the case of a tie, the winner(s) will be selected based on the highest votes from the judges.
In the event that none of the submissions meet the Judging Criteria, the sponsor will award the following consolation prizes to the competitor that score the highest:
- Consolation Prize 1: $3000
- Consolation Prize 2: $1000
Judging Panel
The determination of the winners will be made by a group of proven experts, including Prof. Dr. med. Philippe Schucht, HORAO project manager.
Additional Information
- By participating in the challenge, each competitor agrees to submit only their original idea. Any indication of «copying» amongst competitors is grounds for disqualification.
- All applications will go through a process of due diligence; any application found to be misrepresentative, plagiarized, or sharing an idea that is not their own will be automatically disqualified.
- All ineligible applicants will be automatically removed from the competition with no recourse or reimbursement.
- No purchase or payment of any kind is necessary to enter or win the competition.
- Void wherever restricted or prohibited by law.
The text above is also available as PDF: Guidelines (PDF)